Listen to this article
The NHS waiting list has recently reached its lowest level in nearly three years, bringing a glimmer of hope amid ongoing concerns about hospital waiting times. With 7.29 million patients awaiting essential treatments by December 2025, progress has been evident; however, challenges remain, particularly in A&E departments where record 12-hour trolley waits have been reported. This alarming statistic highlights the ongoing pressure on healthcare services, even as NHS updates suggest a path to recovery. The Health Secretary has acknowledged this significant progress while also warning of the work still ahead to ensure timely care. As the nation looks to overcome these hurdles, the focus remains on improving NHS recovery progress and addressing the disparities in patient experiences across the country.
The issue of NHS waiting lists, often referred to as treatment backlogs, has become a critical topic in discussions about public health. Patients are frequently facing prolonged waiting times for surgeries and consultations, affecting their overall health outcomes and well-being. Moreover, emergency care, particularly in emergency departments, continues to be strained, resulting in some patients experiencing long waits for hospital beds. This situation underscores the challenges facing accident and emergency services amidst ongoing efforts to enhance healthcare delivery across the NHS. As authorities strive to stabilize these pressing issues, it is essential to monitor the effectiveness of ongoing reforms and the impact they have on patient care.
The Current State of NHS Waiting Lists
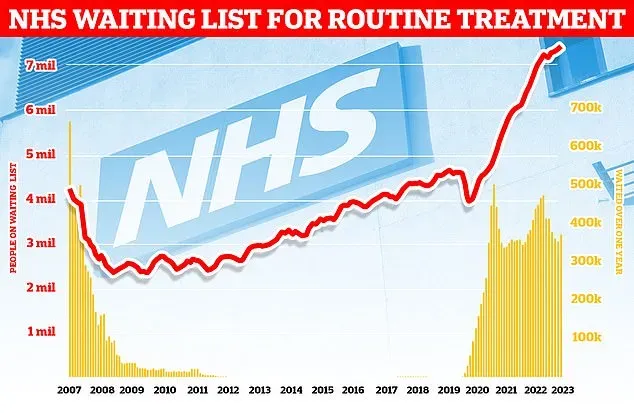
As of December 2025, NHS waiting lists in England have significantly improved, marking the lowest number of patients waiting for treatment in nearly three years. With 7.29 million patients awaiting procedures such as knee and hip operations, it signals a positive trend in the NHS’s ability to manage and reduce backlog. Hospital officials laud this milestone as a result of ongoing efforts to streamline healthcare services and improve patient care amid broader challenges within the system.
Despite this progress, the NHS continues to face lingering issues, particularly in Accident & Emergency (A&E) departments. Prolonged A&E waiting times remain a pressing concern, evidenced by a record number of patients enduring over 12-hour waits in January 2026. This situation highlights the complexities of managing patient flow in hospitals, as many A&E visitors, especially the elderly and those requiring more intensive care, are placed at risk due to constrained facilities.
NHS Recovery Progress and Ongoing Challenges
Health Secretary Wes Streeting acknowledged the advancement made by the NHS while simultaneously emphasizing the need for continued improvements. Addressing the current NHS recovery progress, he stated, “There is much more to do. We’ve got to pick up the pace… but the NHS is on the road to recovery.” This recognition of progress juxtaposes the challenges that still threaten the system, such as staffing shortages and the need for infrastructure improvements to support recovery.
The NHS Confederation’s Rory Deighton highlighted the inconsistencies in healthcare delivery across various regions in England. Although the overall reduction in waiting lists is commendable, disparities exist among different hospitals, which complicates efforts to address care backlogs uniformly. Such variations stress that while the NHS aims for national standards, regional operational challenges can hinder patient care progress.
The Impact of A&E Waiting Times on Patient Care
Waiting for treatment in A&E has substantial repercussions on both patient outcomes and healthcare provider resources. The recent data revealing that over 71,500 patients faced extended waits of more than 12 hours indicates a troubling trend that could affect patient health adversely. Long waits not only strain the capacity of emergency services but also diminish the quality of care received by vulnerable populations.
As noted by Dr. Vicky Price of the Society for Acute Medicine, operating beyond capacity is a clear indicator that the NHS is under distress. Patients requiring emergency care, particularly older individuals with complex needs, face the greatest risk when hospitals cannot provide immediate assistance. Thus, addressing A&E waiting times is crucial for ensuring that the NHS can meet its commitment to safeguarding patient health and maintaining service efficiency.
Regional Variations in NHS Performance
One major takeaway from the latest NHS updates is the acknowledgment of substantial regional variations in performance across England’s healthcare system. These differences can significantly impact patient care and the effectiveness of recovery strategies. While some areas report remarkable improvements in hospital waiting times and service delivery, others struggle with chronic backlogs and insufficient healthcare resources.
Duncan Burton, Chief Nursing Officer for England, noted that even amidst a backdrop of substantial progress, each hospital functions in its unique context characterized by distinct financial and operational challenges. This regional disparity underscores the importance of tailored strategies and resource allocation to ensure equitable access to healthcare services across different communities.
Government Goals for NHS Improvement
The government has set ambitious targets to bring NHS waiting times back in line with national expectations, with an eye towards the 18-week target by 2029. Currently, only 61.5% of patients are seen within this timeframe, a slight decline from previous months, reinforcing the need for strategic planning to enhance healthcare service efficiency. Meeting these targets is critical not just for patient satisfaction but for restoring public trust in the NHS.
While the reduction in waiting lists marks progress, the government acknowledges that sustaining this momentum requires addressing the underlying causes of delays. This includes investing in healthcare workforce training, expanding facilities, and improving management practices to better handle patient influx, particularly in A&E settings. By aligning efforts across various fronts, the NHS aims to solidify its recovery path and enhance overall patient care quality.
Staffing Challenges Amidst NHS Recovery
NHS staffing has been and continues to be a significant barrier to recovery and service delivery. The impact of recent strikes by junior doctors has led to an intensified focus on the importance of healthcare workforce stability. The government’s strategies must not only aim at reducing waiting lists but also prioritize bolstering staff morale and addressing recruitment and retention to allow for adequate staffing levels.
Duncan Burton praised the dedication shown by health workers throughout these turbulent times, noting that despite the circumstances, notable reductions in patient waiting lists were achievable. Moving forward, it will be essential for health leaders to foster an environment that supports staff well-being and professional growth, ensuring that the NHS has the capacity to meet the increasing demands placed upon it.
Public Perception and Trust in the NHS
Public trust in the NHS remains crucial as the organization navigates recovery and attempts to address current challenges. The alarming figures related to A&E waiting times can lead to a decline in public confidence among patients relying on these vital services. Ensuring transparency about efforts to tackle these issues and honest communication regarding challenges is key to restoring trust.
Furthermore, enhancing patient engagement by allowing families and patients to voice their experiences plays a pivotal role in improving NHS services. The incorporation of feedback into operational strategies can provide valuable insights, enabling the NHS to tailor its healthcare services better and effectively address patient concerns moving towards future recovery.
The Future of NHS Healthcare Services
Looking ahead, the future of NHS healthcare services will depend largely on the ability of the system to adapt to changing patient needs and external pressures. Innovations in healthcare delivery, including telemedicine and outpatient services, may serve to alleviate some of the pressures currently facing A&E departments and reduce overall hospital waiting times. Equipping healthcare facilities with modern technology can increase efficiency and improve service quality.
Moreover, ongoing collaboration between health organizations, government agencies, and community stakeholders is vital for creating a more resilient NHS. As healthcare demands evolve, the establishment of agile, patient-centered care models will be necessary to ensure that the NHS can navigate future uncertainties while providing high-quality care to all patients.
Comprehensive Strategies for NHS Improvement
To address the significant challenges currently facing the NHS, comprehensive strategies centered on operational excellence, strategic staffing, and financial stability will be essential. These strategies should prioritize immediate operational improvements while also planning for long-term sustainability within the system. This dual approach will help mitigate waiting list pressures and maintain service quality.
Additionally, increasing community health initiatives and preventive measures can contribute to lowering hospital admissions, further alleviating pressure on both A&E departments and elective surgeries. A concerted focus on public health will be necessary to create a more sustainable NHS that is equipped to handle future demands and continue its recovery progress.
Frequently Asked Questions
What is the current status of NHS waiting lists as of early 2026?
As of January 2026, NHS waiting lists have dropped to 7.29 million patients, the lowest level since February 2023. This reduction highlights ongoing recovery in NHS healthcare services.
How do NHS hospital waiting times compare to A&E waiting times?
While NHS hospital waiting times have seen improvement, A&E waiting times remain a concern, with a record number of patients experiencing lengthy waits for treatment, indicating challenges in emergency care.
What factors are contributing to the NHS recovery progress regarding waiting lists?
The NHS recovery progress is attributed to effective staff dedication and ongoing investments, even amidst challenges like strikes. However, performance against the target for treating patients within 18 weeks remains below expectations.
What are the long-term targets for NHS waiting lists?
The government aims to meet the 92% target for treating patients within 18 weeks by 2029, despite current statistics showing only 61.5% achieving this benchmark in recent reports.
What does the NHS say about regional variations in hospital waiting times?
The NHS acknowledges significant regional variations in hospital waiting times, which complicates efforts to address healthcare backlogs, as different areas face unique operational challenges.
What measures are being taken to improve NHS hospital waiting times?
NHS updates suggest ongoing monitoring, resource allocation, and strategic planning are crucial for improving hospital waiting times while enhancing healthcare services across different regions.
How does the NHS ensure safety during prolonged A&E waiting times?
NHS officials emphasize the importance of maintaining patient safety during prolonged A&E waiting times, especially for vulnerable populations at risk due to excessive waits.
What recent developments have occurred regarding NHS A&E waiting times?
Recent NHS updates reveal that over 71,500 patients faced waits exceeding 12 hours in A&E, highlighting critical challenges in timely care delivery within emergency services.
How can patients stay informed about NHS waiting lists and updates?
Patients can stay informed about NHS waiting lists and updates through official NHS communications, local healthcare service announcements, and media reports on hospital performance.
What steps is the NHS taking to address the backlog caused by waiting lists?
To address the backlog, the NHS is focusing on enhancing operational efficiency, increasing staff availability, and utilizing technological solutions to streamline patient processing and care.
| Key Point | Details |
|---|---|
| Current Waiting List Status | 7.29 million patients are currently waiting for treatments, the lowest since February 2023. |
| A&E Waiting Times | Over 71,500 patients waited more than 12 hours for a bed in January 2026, the highest since 2010. |
| Health Secretary’s Statement | Wes Streeting acknowledged progress but emphasized ongoing challenges in the NHS. |
| Hospital Safety Concerns | Hospitals are reported to be operating beyond safe levels, raising risks for vulnerable patients. |
| Performance Against 18-Week Target | Only 61.5% of patients waited less than 18 weeks, down from 61.8% in November 2025. |
| Regional Variations | Responses to care backlogs vary across different areas, complicating overall improvement efforts. |
Summary
The NHS waiting list has seen a significant decrease to its lowest level in three years, indicating progress in patient treatment times. However, challenges remain, particularly in A&E where record waiting times persist, highlighting the need for continued improvement and targeted solutions. The government’s pledge to meet the 18-week target by 2029 remains a focal point amid ongoing issues in emergency care, underscoring the complexity of the NHS landscape.